Here are a selection of articles written by Dr M K Vasant, which were published in professional dental journals.

by Dr M K Vasant MBE BDS, MGDS, FFGDP(UK), FDS RCS, Dip T Ed is a practitioner in London. A specialist in prosthodontics, he is also a diploma tutor for the central London division of the FGDP and lead advisor in vocational training for the University of London.
In the light of last year's OFT report, Manny Vasant outlines his vision of private dentistry.
Dentistry is predominantly a primary care profession. 95% or more of all dentistry is undertaken in the primary care sector; 90% of the dental manpower is employed in the primary dental care sector. Each primary care practitioner runs effectively a mini-hospital with all required tools to support comprehensive treatment for patients (RajaRayan, 2002). The majority of current dental practitioners in the UK have practiced under the General Dental Services of the NHS. Many are still mixed practices, albeit, with an increasing shift towards private practice. It is a small wonder that the standards vary from practice to practice. It is generally accepted that the primary reason for the shift towards private dentistry is to escape third party interference so that a clinician may provide the best care for his/her patient at a reasonable fee. There is common perception amongst GDPs that the NHS fees are unrealistically low to be able to practice the type of dentistry that one is taught
There are tales of practitioners turning 'private' overnight. The act of 'going private' in some quarters merely implies the change of a price list! This is unethical, unjust and deceitful. I hasten to add, that there are a number of practitioners who, against all adversity, practise very good quality of dentistry under the GDS. They must work extremely long hours and are of 'super breed' variety. Conversely, there are private practices whose standards leave much to be desired; unlike in the general dental services, there is no equivalent to the 'Big Brother' - the dental reference officers of the Dental Practice Board. Hopefully journals such as this one fill the gap and allow private practitioners to undertake a self-evaluation on one's own practice. Perhaps through these journals one would hear a voice saying 'mind the gap' (excuse the pun!).
If the reasons for the change have been interpreted correctly, private dentistry must be about raising standards and providing unrestricted best professional care. Amongst the standard-setting bodies in the UK is the Faculty of General Dental Practitioners (FGDP), whose raison d'etre is to raise standards in general dental practices. It is reasonable to assume that a private practitioner measures his or her performance against this yardstick. Using FGDP guidelines and protocols (see publications in references) and that of other bodies such as the General Dental Council, the British Dental Association, specialist societies, BUPA and Denplan (to name a few), one's practice must evolve over a period of time. It is expected that by removing financial and other constraints, one would be able to deliver better quality of care in a more convivial environment. In an ideal world, the same standards must apply to all practices, but given the current constraints in the GDS fees, this must be difficult to attain.
Perhaps the easiest way to look at one's private practice is through the Donabedian concept of structure, process and outcome. This concept is used in industry for quality control and also by the FGDP (UK) in the assessment for the Fellowship Diploma (FFGDP) to measure the quality of care provided. This concept also paves the way for clinical governance currently promulgated by the government.
This is related to a provision of facilities, equipment, and organisation that are evident, and to the training, qualifications, numbers and attributes of personnel
Naturally, the layout of an existing practice is not easily amenable to change, although an opportunity to relocate to nearby premises or acquiring/building additional space should be considered if at all possible. The reception area and patient lounge, (rather than waiting area) must fulfil higher expectations of the patients, as should the treatment rooms. Patients expect current magazines targeted to different age groups and interests to be available in the lounge. Patients also expect to receive information on dentistry and need to be educated about various treatment modalities. Our practice has found it very beneficial to have a 42-inch plasma screen (Figure I), which continuously plays dental educational programmes. There are several high quality programmes commercially available. We have also linked our website to this and made the programme interactive. This will enable a patient to watch a two minute presentation on flossing, porcelain veneers, tooth whitening or any other treatment modality. There is also a section dedicated for young children involving a dog's family and a monkey visiting a dentist. Although the programme is intended
Furthermore, the screen also has flashing messages with various 'notices' asking patients to report changes of address, telephone numbers and medical history. This medium is an extremely effective way of delivering these messages.
The equipment should be modern, comply with current health and safety standards and be capable of efficient disinfection. There should be no hazards to patients or staff and minimalist equipment/items on work surfaces. This is not only to avoid clutter but is more aesthetically pleasing and less threatening to patients. It also prevents aerosol spray from the handpieces contaminating these items. Needless to say, an adequate number of instruments will ensure that one does not need to wait for them to be sterilised between each patient. Provision must also be made for a back-up autoclave. A log of servicing should be kept adjacent to each machine. The radiographic equipment is also maintained on a regular basis with a log readily available to see.
The single most important piece of equipment that I consider indispensable for practicing good dentistry (especially for a middle-aged dentist like myself), is a set of magnification loupes and accompanying illumination - a 'private' vision so to speak! I feel this changes one's perception of dentistry and goes hand in hand with photography. This also opens one's eyes because it lends oneself open to scrutiny.

If private dentistry equates to better quality of care then one must accept that one has to be equipped with adequate and contemporary information and techniques. This means continuing professional development and possibly peer review. Ideally this means acquitting oneself in a postgraduate diploma such as those made available by the Faculty of General Dental Practitioners (UK).
Depending on the size of the practice, an adequate number of clinical and administrative staff are needed to cope with the increased expectations and needs of private patients. More importantly, a training programme for the staff must be in place. This is probably the most overlooked aspect in practices. In its recent reforms, the General Dental Council has placed much greater emphasis on training the team.
Our practice has greatly benefited from various staff manuals, in-house training and the resultant protocols that have been put in place (Figure 2). They have been invaluable in the day-to-day running of the practice and have enhanced staff morale and patient satisfaction.
The staff manual gives all essential information about the practice. The sections include:
We produced our first manual over 20 years ago and this is the third edition. Each treatment room (we are a five-surgery practice with four full-time dentists and two part-time hygienists) has a copy for reference. To supplement this, another manual called System Operating Procedures (SOP), has instructions on using the electronic credit card machine, telephone systems etc.
We have found a unique way of ensuring that staff (especially new staff) read this manual. After all, many practices do have such manuals but find that staff do not read them! Each staff is given a folder called the personnel development portfolio. This portfolio was produced in conjunction with staff and associates about seven years ago. The portfolio contains five modules. Each module is effectively a 'syllabus' of what we expect the staff to know after one, three, six, twelve and eighteen months in practice.
For example, in the first month of taking employment we will simply need them to know:
The three-month module gets a little more detailed - for example, we would expect them to know what drugs are in the emergency box and so on. At the end of the appropriate period there is an assessment of the knowledge. The MCQs can be answered at home or by reading the staff manual, which contains all the required information. Assistance from senior colleagues is also encouraged. Then the nurse/receptionist has to present himself/herself for a viva voce for lO minutes. The viva voce is conducted by senior nurses/associates who will then give a certificate for the module satisfactorily completed. If any aspect is not satisfactorily completed, the candidate is asked to return a week or two later once he/she has learnt the relevant procedure/subject. The viva voce will include tests such as printing out dental treatment plan as prescribed by the dentist, making an appointment on the computer or finding a specific leaflet. The pay rise and various other promotions are linked to the completion of this assessment. Employees seem to be in a hurry to complete this!
Once they complete the fifth module (which is similar in syllabus to the National Board for Dental Nurses examination), they are encouraged to sit the Dental Nurses examination. We have found this invaluable. We have found that as all staff have ownership of this manual, they wish to get actively involved.
The PDP remains the property of the staff and if they leave the practice, they take the POP with them. This is very useful for the new employer because they have a record of the procedures that the interviewee is capable of performing.
Needless to, say, a private practice must have access to a good laboratory able to meet higher expectations of the patients. In order to maintain consistency and quality with dental technicians, a laboratory manual has been produced. The information given out here is to enhance the prescriptions for various procedures. New or junior staff in the laboratory find this invaluable. There are also illustrations of problems either borrowed from textbooks or actually experienced by us. For example, one photograph graphically shows how a partial coverage splint can result in an anterior open bite - not an uncommon scenario for bleaching trays and post orthodontic retainers! This manual augments prescriptions written for each case and helps to avoid any recurrent problems and perhaps repetition in laboratory prescriptions.
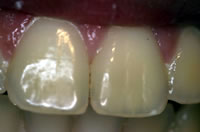
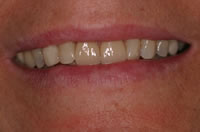
Naturally, a private practitioner and patients alike would expect attention to detail in the restorations produced. For example, where necessary, technicians are encouraged to copy contours (lobes) of labial surfaces of natural central incisors (Figure 3) to mimic natural dentition during manufacture of restorations (in this example porcelain veneers on 1|1 (Figure 4) so that light reflection mimics that of a natural dentition.
As would be expected, the CPR is regularly taught and practiced in the surgery. The dentists/hygienists are required to go on CPD and once a week the dentists/hygienists meet up over lunch to 'talk shop'.
Patient records are maintained on the computer and there is also a manual record card for each patient. Personnel are trained to maintain quality of the records as per guidance in Clinical Record Keeping (FGDP). It is intended that manual record cards will be dispensed with, once radiographs have been digitised. At the moment the manual record wallet contains radiographs and various other forms. Admittedly, although the practice has successfully used surgery-based dental software for six years, the
Each patient is also telephoned the day before to confirm the appointment booked. This reduces the 'no-shows' to almost nil.
What the dentist and his/her team actually do in the delivery of care includes all aspects of management from history taking to the technical procedures of treatment.
All new patients or patients returning after an absence of two years are required to have a full case assessment. The fee for this assessment is publicised on the website and quoted over the telephone. A pro-forma is completed during this examination in order to be assured that hard tissues, soft tissues, periodontal tissues are adequately examined and recorded. Obviously, medical history is also updated and questions asked about smoking habits and alcohol consumption.
Necessary radiographs are taken, in keeping with the guidelines contained in Selection Criteria for Dental Radiography (FGDP). hi order to enhance the quality of information gleaned from intraoral radiographs, a light box with black cardboard background and a suitable window cut out to accommodate an intraoral radiograph is available. The problems are fully discussed with the patient by using an intraoral camera where necessary. Different options are discussed. The intraoral camera, as we know, highlights the smoker's stains on teeth. Therefore, it presents an ideal opportunity to enter into smoking counselling.
The photographs are often given to patients, along with written treatment plans with options and costs so that they can discuss the proposals with their spouses and return for further discussion with further questions. This is computer generated and in most cases also supplemented with a hand written' discussion' sheet. The latter is in the form of NCR paper (No Carbon Reproduction) which produces two copies. It contains drawings and/or any comments made about the condition or treatment proposed. This is an excellent medico-legal document and a fantastic communication tool that significantly enhances the computer printout. A signed copy is retained in the file and the top copy is given to the patient.
Ample written educational material is available for patients to enhance their treatment plans. This information is also freely available on the practice website. Where advanced restorative care is planned, patients will also receive the Guide to Success and Survival of Restorations. This document came out as a result of an audit project that was carried out when it was felt that the practice lacked some information that could be given to the patients, for example, on longevity of the new ceramic crowns. Rather than write this in each treatment plan, it was found much more convenient to list various restorations on one sheet and give prognosis based on research studies published. This has proven to be very popular and is administratively very cost effective.
Where referrals to specialists are necessary, this is done either by writing a letter on computer or using a purpose-made NCR form. The latter is extremely efficient as the chair-side staff is trained to fill in the relevant parts whilst the discussion is going on with the patient. The design of the letter allows it to be folded and placed in a window envelope thus minimising the work involved. A copy is retained in the records. The practice protocols require such letters to be given to patients at the same visit to save collecting a backlog of paperwork afterwards.
How we measure the status, benefit, knowledge and satisfaction
From time to time a survey is conducted amongst patients to measure satisfaction levels and invite any criticisms. The plasma screen also has flashing messages, which, amongst other things, informs patients of the complaints/suggestions procedure.
Patients are recalled at six-monthly intervals and the examination starts with a review of the last course of treatment. Any treatment that warrants retreatment is carried out free of charge within the first year and then for a further two to three years at the discretion of the dentist.
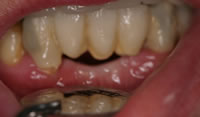
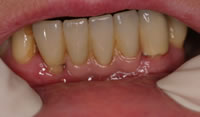
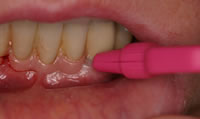
First and foremost is patient satisfaction. Where necessary, before and after photographs are given to the patient illustrating what their treatment has achieved (Figures 5 & 6). Care is also taken to ensure that the patient understands the maintenance procedures for these restorations (Figure 7).
The second aspect (which is equally important for quality care) is peer review to share information and attain the best outcome for the patient. It must be recognised that the most expensive treatment is not necessarily the best care for the patients. The two examples below from our practice illustrate the principle.
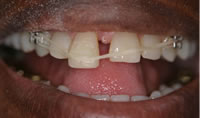
Figures 8 & 9 illustrate how a simpler and much cheaper form of treatment (the patient will have a bonded lingual retainer when appliance is removed in a week's time) was a better option in this case. Similarly, a simple feldspathic resin dentine-bonded ceramic crown is a far less invasive, cheaper and a very aesthetic solution. One does not have to choose the most expensive crown from the laboratory price list for a private patient!
It is appreciated that good practices will vary in style and delivery of care. However, the principles of structure, process and outcome as a measure of good practice must be the same.

Same patient six weeks later following simple periodontics and orthodontics (two brackets with elastic retained with a blob of composite on 1| for intrusion and retroclination)
In writing this article I cannot overemphasise the other three most important requirements for raising one's standards. These are education, education and education for the team! This must go hand in hand with the structure, process and outcome. I hope I have succeeded in establishing that private dentistry must be synonymous with a raised standard of care and that the key issue is education for the team.
Burke FJT, Watts DC (1994).
Fracture resistance of teeth restored with dentin-bonded crowns.
Quint Int 25: 335-340
Office of Fair Trading (2003).
The Private Dentistry Market in the UK.
July 2003 www.oft.gov.uk
RajaRayan R OBE (2002).
Standing on Shoulders of Giants
A consultation document on future direction of the Faculty of General Dental Practitioners (UK)
The following FGDP publications are obtainable from 35-43 Lincoln's Inn Fields London WC2A 3PE. Tel 020 7869 6754 or visit www.rcseng.ac.uk

